Dr. Kennan T. Runte, DPM, FACFAS
Dr. Panah Nabili, DPM
Grass Valley, CA 95945
Dr. Kennan T. Runte, DPM, FACFAS
Dr. Panah Nabili, DPM

Debilitating foot pain is a problem for many people. But just as stretching the torso can help alleviate back pain, stretching the feet can also help mend existing foot problems and prevent future ones.
The feet, as the body’s foundation, carry the body’s entire weight and can get easily strained from overexertion. Persistent sharp pain and cramping in the feet are often common concerns. Foot pain and foot problems can be due to any number of causes, and in many cases pain may be eased without medication or doctor visits. It is always a good idea, however, to first rule out any serious medical issues with a physician.
Stretching can help relax the feet and alleviate pain, but is especially important before heavy aerobic exercise. Stretching before such activities can help you avoid experiencing painful cramps or strained foot muscles. Stretches should be performed slowly and deliberately without forceful pulling. The stretch should be held for several seconds before relaxing.
A great way to stretch out and loosen up the foot muscles while sitting is to cross one leg over the other and pull the toes carefully back without overextending. Start by resting the left ankle on the right knee. With the left hand, gently flex the left foot by pulling back on the toes. Do not pull too hard; just hard enough to feel the stretch in the arch of the foot. Then point the toes of the left foot as far as you can. Rotate the motion of pointing with pulling back on the toes. This should relax and stretch the muscles on the bottom and the top of the foot. Doing this stretch ten to twenty times should bring relief. Repeat the whole process for the other foot by resting the right ankle on the left knee.
A stretch that focuses on the often injured Achilles tendon involves standing and facing a wall with your arms out and hands flat against the wall. Step back with one foot, keeping it flat against the floor. Move the other leg forward and lean toward the wall. You should feel a stretch through the back of your leg and your Achilles tendon, but do not push yourself too much. Stop when you feel a stretching sensation, and hold for 30 seconds. Ten repetitions may be done for each foot.
Stretching the feet is important for athletes or those performing aerobic exercise, but it can also help anyone with foot pain caused by poor footwear, plantar fasciitis, or long hours standing and walking. Individuals who tend to their feet by regularly stretching every day should be able to minimize foot pain and prevent new problems from arising.
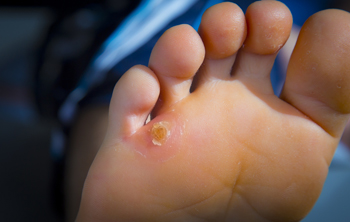 Corns are small, circular, thickened areas of skin on the feet that have a central core of hard material. They get their name due to their resemblance to a kernel of corn. Corns are caused by repeated pressure on the skin, usually from shoes rubbing against the area. They can form on the soles of the feet, the tops of the toes, or in between the toes. Usually, the corns that form in between the toes are softer than those that form elsewhere on the foot. If you have corns that are causing pain or discomfort, a podiatrist can help treat them. The doctor may suggest changes to your footwear, prescribe orthotic inserts, or remove the thickened skin. For more information about corns on the feet, please speak with a podiatrist.
Corns are small, circular, thickened areas of skin on the feet that have a central core of hard material. They get their name due to their resemblance to a kernel of corn. Corns are caused by repeated pressure on the skin, usually from shoes rubbing against the area. They can form on the soles of the feet, the tops of the toes, or in between the toes. Usually, the corns that form in between the toes are softer than those that form elsewhere on the foot. If you have corns that are causing pain or discomfort, a podiatrist can help treat them. The doctor may suggest changes to your footwear, prescribe orthotic inserts, or remove the thickened skin. For more information about corns on the feet, please speak with a podiatrist.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact one of our podiatrists of Foothill Podiatry Clinic. Our doctors will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Grass Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns are hard and thick areas of skin that form as a result of constant rubbing, friction, or pressure on the skin. They are patches of dead skin with a small plug toward the center. They may appear on the tops and sides of toes and can make walking painful.
Soft corns are typically thinner with a white color and rubbery texture. Soft corns tend to appear between the toes. Seed corns are another type of corn that appear in clusters and can be tender if they are on a weight-bearing part of the foot. Seed corns usually appear on the bottom of the foot and are likely caused by a blockage in sweat ducts.
While corns and calluses are somewhat similar, calluses are a bit different. Calluses are a patch of dead skin that can occur anywhere on the body. In comparison to corns, calluses are usually a bit larger in size. However, both corns and calluses are caused by increased friction on the skin.
There are some risk factors that may increase your chances of developing corns and calluses. If you have bunions, hammertoe, or a bone spur, you are more likely to develop a corn or callus on your foot.
While Corns and Calluses tend to disappear when the friction to the affected area ceases, the help of a podiatrist may be useful in the removal process. It is important to remove the dead skin around the area and this may be done in a few different ways. Moisturizing creams may be helpful in softening and removing the dead skin around the callus. You should never use razors or other pedicure equipment to remove your corns. Doing this may worsen your corn or callus and cause infection.
In some cases, corns and calluses may be caused by abnormal foot structure or walking motion. In such a case, you should seek a podiatrist’s assistance in order to correct the issue.
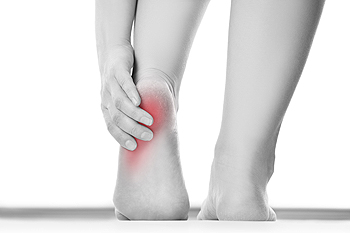 The calcaneus, or heel bone, and its supporting fat pad, tendons and ligaments bear the brunt of the body’s weight and impact, while absorbing the stress of walking and running. For this reason, it is not uncommon for people of all ages and lifestyles to develop heel pain. Children and adolescents can develop Sever’s Disease when the growth plate of the calcaneus is repeatedly stressed due to growth spurts or physical activity. Plantar fasciitis (inflammation of the tissue on the bottom of the foot from heel-to-toe) and Achilles tendonitis (inflammation of the tendon connecting the calf muscles to the heel bone) can occur at any age, but is most common among adults. Whatever your lifestyle or age, contact a podiatrist if you or someone you love is experiencing any type of heel pain.
The calcaneus, or heel bone, and its supporting fat pad, tendons and ligaments bear the brunt of the body’s weight and impact, while absorbing the stress of walking and running. For this reason, it is not uncommon for people of all ages and lifestyles to develop heel pain. Children and adolescents can develop Sever’s Disease when the growth plate of the calcaneus is repeatedly stressed due to growth spurts or physical activity. Plantar fasciitis (inflammation of the tissue on the bottom of the foot from heel-to-toe) and Achilles tendonitis (inflammation of the tendon connecting the calf muscles to the heel bone) can occur at any age, but is most common among adults. Whatever your lifestyle or age, contact a podiatrist if you or someone you love is experiencing any type of heel pain.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of Foothill Podiatry Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Grass Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Peripheral Artery Disease (PAD) is a restriction of blood flow to the muscles and organs due to the build-up of plaque on artery walls. PAD starves muscles and organs of the oxygen and nutrients they need to function properly—especially during physical activities. This lack of oxygen-rich blood to the extremities can make it difficult to walk and can also cause pain in the feet and legs. This pain from PAD can go undetected in people who also suffer from diabetes and neuropathy, possibly leading to foot sores which—when caused by severe blood flow reduction—can increase the risk of amputation. Individuals who are afflicted with PAD and/or diabetes should be under the care of a podiatrist who can help to manage these conditions and improve overall health.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with one of our podiatrists from Foothill Podiatry Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our office located in Grass Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
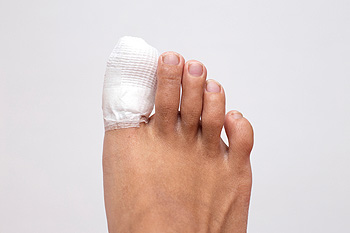 Broken toes are often a result of something being dropped on it, stubbing it, or bending it the wrong way. Broken toes are often indicated by a snap or popping sound when the injury occurs, swelling, bruising, deformity, decreased movement, and worsening pain when the toe is moved or touched. Patients who believe that they have broken their toe should consult with a podiatrist for a proper diagnosis. A podiatrist will check the toe and may need to take an x-ray. Once the broken toe has been diagnosed, the podiatrist will choose the treatment option that is best for the particular injury. Depending on the severity of the break, the toe may be “buddy-taped” to the uninjured toe next to it. A cast, splint, or brace may also be used to treat the toe, and in severe cases, surgery may be necessary.
Broken toes are often a result of something being dropped on it, stubbing it, or bending it the wrong way. Broken toes are often indicated by a snap or popping sound when the injury occurs, swelling, bruising, deformity, decreased movement, and worsening pain when the toe is moved or touched. Patients who believe that they have broken their toe should consult with a podiatrist for a proper diagnosis. A podiatrist will check the toe and may need to take an x-ray. Once the broken toe has been diagnosed, the podiatrist will choose the treatment option that is best for the particular injury. Depending on the severity of the break, the toe may be “buddy-taped” to the uninjured toe next to it. A cast, splint, or brace may also be used to treat the toe, and in severe cases, surgery may be necessary.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact one of our podiatrists from Foothill Podiatry Clinic. Our doctors will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions, please feel free to contact our office located in Grass Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
A broken or fractured bone in the foot is not always obvious. While it may cause symptoms such as pain, swelling, bruising, and difficulty walking, your doctor will still need to perform certain tests in order to confirm the diagnosis. X-rays, CT scans, bone scans, or an MRI can all be used to visualize the broken bone, as well as other foot injuries. If a bone in the foot is broken, a podiatrist may prescribe a variety of treatments depending on the severity of the break. These may include modifying daily activities to reduce stress on the affected foot, wearing a cast or splint, or surgery. If you suspect that you may have broken your foot, please seek the care of a podiatrist as soon as possible.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Foothill Podiatry Clinic. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our office located in Grass Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.